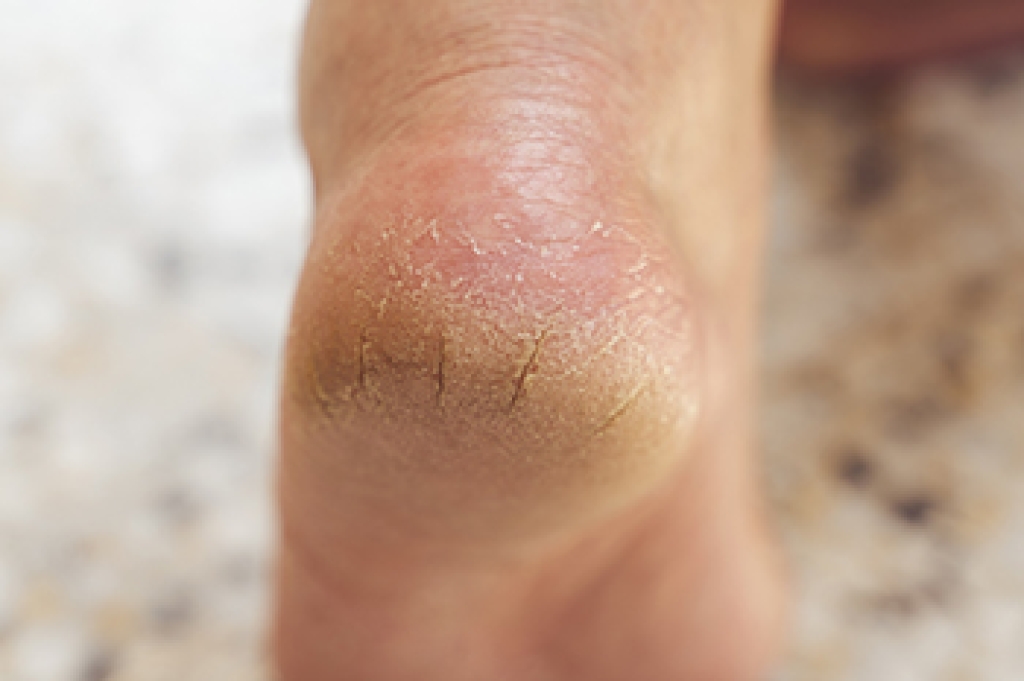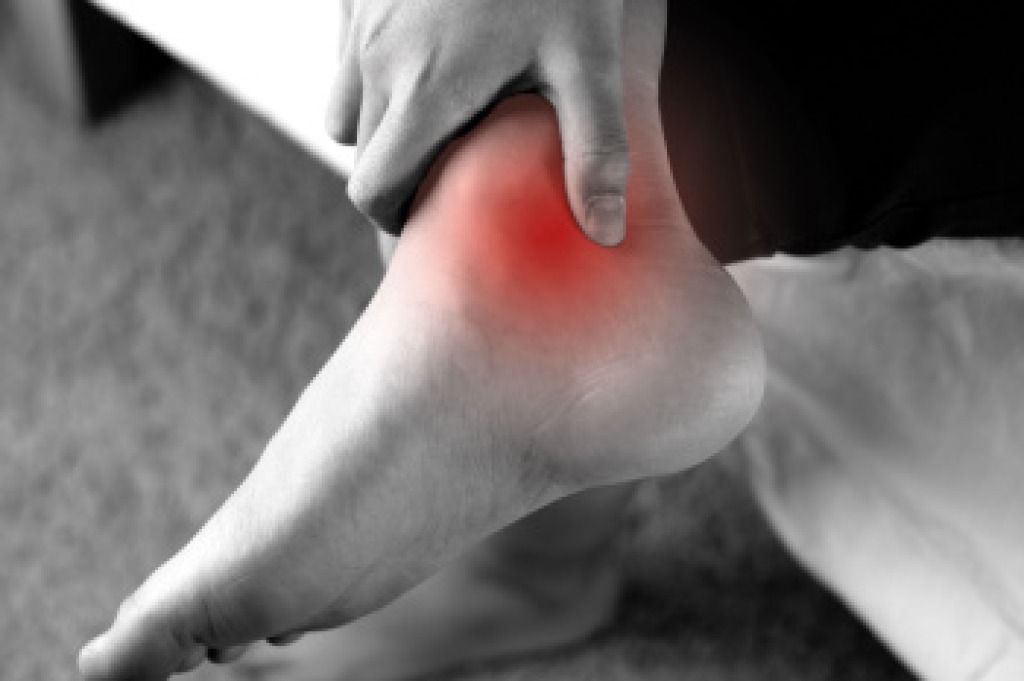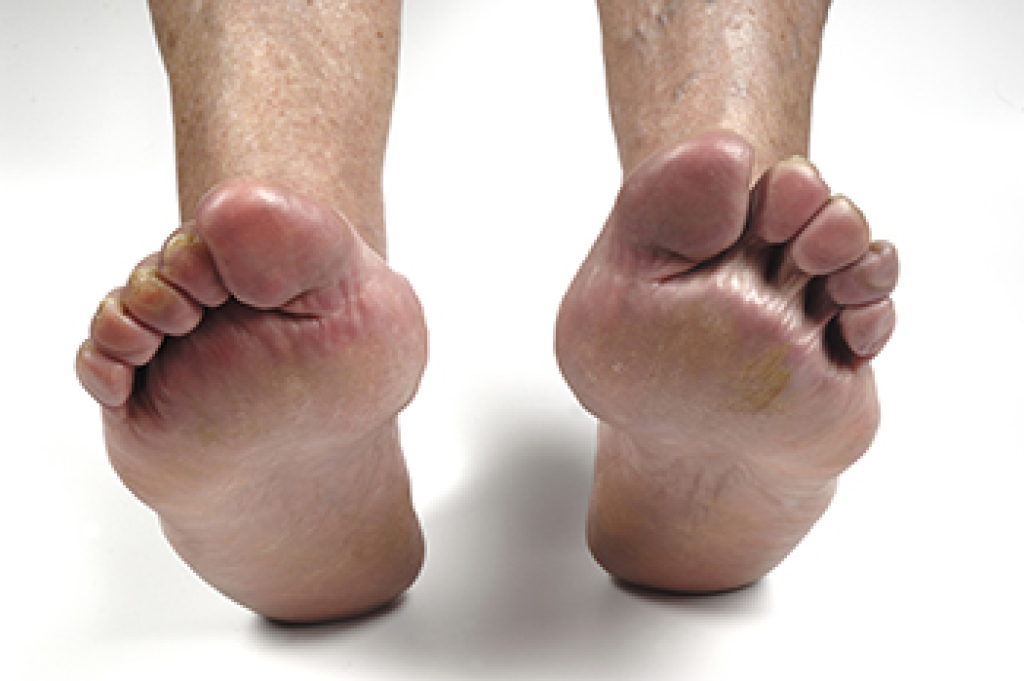
Rheumatoid arthritis is an autoimmune condition that causes the body to mistakenly attack its own joints, and the feet are often among the first areas affected. Inflammation can lead to swelling, stiffness, and a deep aching sensation, particularly in the toes and the ball of the foot. Over time, the joints may shift or lose stability, making walking uncomfortable and sometimes altering the shape of the foot. Many individuals also notice warmth, tenderness, or difficulty standing for long periods. Because these changes can progress gradually, early attention is important to protect mobility and reduce strain on surrounding joints. Supportive footwear, gentle exercises, and timely care all help manage symptoms more comfortably. If you have persistent swelling, stiffness, or joint pain in the feet, it is suggested that you schedule an appointment with a podiatrist for further evaluation.
Because RA affects more than just your joints, including the joints in your feet and ankles, it is important to seek early diagnosis from your podiatrist if you feel like the pain in your feet might be caused by RA. For more information, contact Christian Smith, DPM of UTOEpia Foot and Ankle Specialist. Our doctor will assist you with all of your podiatric concerns.
What Is Rheumatoid Arthritis?
Rheumatoid Arthritis (RA) is an autoimmune disorder in which the body’s own immune system attacks the membranes surrounding the joints. Inflammation of the lining and eventually the destruction of the joint’s cartilage and bone occur, causing severe pain and immobility.
Rheumatoid Arthritis of the Feet
Although RA usually attacks multiple bones and joints throughout the entire body, almost 90 percent of cases result in pain in the foot or ankle area.
Symptoms
- Swelling and pain in the feet
- Stiffness in the feet
- Pain on the ball or sole of feet
- Joint shift and deformation
Diagnosis
Quick diagnosis of RA in the feet is important so that the podiatrist can treat the area effectively. Your doctor will ask you about your medical history, occupation, and lifestyle to determine the origin of the condition. Rheumatoid Factor tests help to determine if someone is affected by the disease.
If you have any questions, please feel free to contact our office located in Memphis, TN . We offer the newest diagnostic and treatment technologies for all your foot care needs.